Keterangan
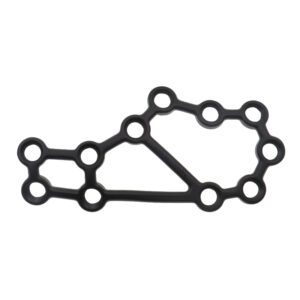
Ankle Fusion Locking Plate
Q&A
Q1: What is an Ankle Fusion Locking Plate used for?
A1: It is used for tibiotalar arthrodesis or tibiotalocalcaneal fusion in patients with severe arthritis, deformity, or instability to provide rigid fixation until bone fusion occurs.
Q2: What are the main types of ankle fusion locking plates and their key differences?
A2: The three primary types are:
Anterior Tibiotalar Plate: Placed through an anterior approach, ideal for isolated tibiotalar fusion with good bone stock.
Posterior Tibiotalocalcaneal (TTC) Plate: Inserted posteriorly, spans tibia, talus, and calcaneus for pantalar or TTC fusion.
Lateral Tibiotalar Plate: Applied laterally, often used when the fibula is preserved or incorporated into the fusion.
The choice depends on bone quality, fusion extent (isolated vs. pantalar), and surgeon preference.
Q3: What material is used for Ankle Fusion Locking Plates?
A3: Typically made from titanium alloy (Ti-6Al-4V) or medical-grade stainless steel, offering high strength, biocompatibility, and radiographic compatibility.
Q4: What types of screws are used with these plates?
A4: The plates use locking screws for fixed-angle stability and often include cortical or compression screws to enhance bone-to-bone contact at the fusion site.
Q5: What are the primary indications for choosing a posterior TTC plate over an anterior plate?
A5: A posterior TTC plate is preferred for:
Significant talar avascular necrosis (AVN) or collapse.
Severe coronal plane deformities.
Revision fusion with poor bone stock in the talus.
Neuropathic arthropathy (misalnya, Charcot foot).
It provides longer screw engagement in the calcaneus for enhanced stability.
Q6: How is patient anatomy accommodated in these plates?
A6: Plates are anatomically contoured for left or right ankles and some allow intraoperative bending to achieve precise adaptation to the patient’s bone.
Q7: What is the typical weight-bearing protocol for each plate type?
A7:Anterior/Lateral Plates: 6–8 weeks non-weight-bearing, gradual progression to full weight-bearing by 12 weeks.
Posterior TTC Plates: 8–12 weeks non-weight-bearing due to longer constructs and poorer bone biology in typical candidates.
Protocols are adjusted based on radiographic fusion progress.